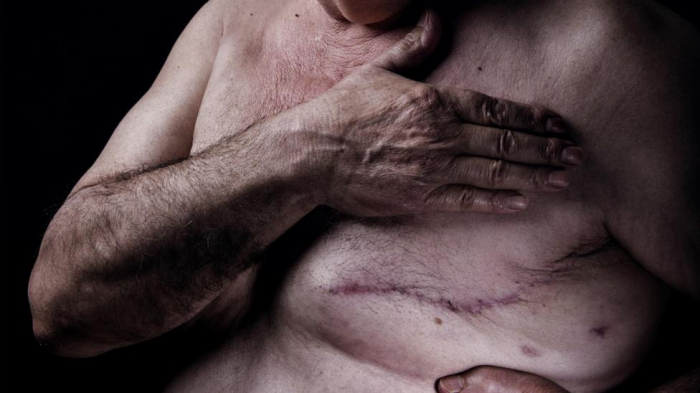
At first, he thought it was just a pulled muscle or heartburn, but when his family encouraged him to do a self-examination, he noticed a number of small, hard bumps that felt like bits of rock candy.
In December 2011, Passanisi, then 66, went for a biopsy at his local hospital in Lake Saint Louis, Missouri, and one day after Christmas, learned those bumps were cancerous. He was diagnosed with stage two breast cancer and was given a single mastectomy with lymphadenectomy a few days later.
“The seatbelt saved his life,” says his daughter Annie Passanisi-Ruggles. The 27-year-old learned a few months after her father’s operation that she carried the same faulty gene that had led to her father’s cancer. The mutation in the BRCA2 gene significantly increases her risk of developing breast and ovarian cancer.
Today, Annie’s on a six month rotation of preventative cancer screenings that include MRIs and mammograms. “If the gene does express, she’ll catch it early,” says Pete.
The BRCA1 and BRCA2 genes are tumour suppressors that are responsible for repairing faults that can naturally occur within DNA. When they do not function correctly, it makes it more likely that other genetic errors will occur, leading to cancer.

Pete Passanisi's diagnosis with breast cancer led his daughter Annie to discover that she too carries the same faulty BRCA2 gene as her father (Credit: Ryan Moore Photography)
Both men and women have the same risk of developing BRCA1 and 2 gene mutations, but men are ten times less likely to get tested for them. One potential reason for this is the general misconception that the genes are synonymous with breast cancer and many men don’t believe they have breast tissue.
Men certainly have less breast tissue than women, which translates to a much lower risk of developing breast cancer even if they have BRCA2 – but that ignores the other risks that come with mutations in this gene.
First, there is the risk it poses to the children of men who carry the faulty gene. Men have a 50% chance of passing down a BRCA2 gene mutation to their children, just as women with the gene mutation do. If their daughters end up inheriting this mutation, they have a 50%-85% chance of developing breast cancer by the age of 70.
“If more men were encouraged to get tested, they’d be helping women [in their families] take preventative measures,” such as regular screenings if they also carry the mutation, says Julie Rani Nangia, director of the Breast Cancer Prevention and High Risk Clinic at Baylor College of Medicine in Houston, Texas.
And it’s not just about how this gene mutation affects women. Male BRCA2 mutation carriers are twice as likely to be diagnosed with prostate cancer in their lifetime than non-carriers, according to one recent study. In fact, 12% of men with metastatic prostate cancer carry a BRCA mutation, which is a higher rate than the percentage of women with breast cancer who carry a BRCA mutation. And prostate cancer in BRCA2 gene mutation carriers is often much more aggressive.

The BRCA1 and BRCA2 genes have become indelibly associated with female breast cancer even though men carry them too (Credit: Getty Images)
“I think we should screen people with prostate cancer for mutations just to avoid the possibility that the surgeon takes a watchful, waiting approach,” says Steven Narod, an oncologist and head of the Familial Breast Cancer Research Unit at the University of Toronto. “You don’t take a conservative approach to prostate cancer in a man with a BRCA gene mutation.”
Only 39% of BRCA2 gene mutation carriers who develop prostate cancer survive to live more than five years after their diagnosis. Depending where you are in the world, the overall five year survival rate of all prostate cancers can vary but it is 84% in the UK and closer to 99% in the US.
Widening the net to identify more men who carry the gene means they can be offered regular testing to identify the early signs that they are developing cancer
There are, however, more effective treatments for patients with the BRCA2 gene mutation than others with prostate cancer. If implemented early, drugs that specifically target cancers caused by these mutations can lead to a more hopeful prognosis.
Widening the net to identify more men who carry the gene means they can be offered regular testing to identify the early signs that they are developing cancer. Ros Eeles, a cancer geneticist at The Institute of Cancer Research in London who oversaw the BRCA2-prostate cancer risk study noted above, is calling for regular blood tests for all men over the age of 40 with faulty BRCA2 genes.
These blood tests can look for raised levels of a protein called prostate-specific antigen, more commonly called PSA, which can indicate that something is amiss in the patient’s prostate. Conducting widespread screening using PSA is difficult because its levels can be raised by a number of conditions including urinary tract infections. But in men carrying a faulty BRCA2 gene, it becomes a powerful tool for detecting a developing tumour.

If more men were tested for BRCA2 mutations, it could raise awareness of the risk they pose and help those with them catch cancers earlier (Credit: Getty Images)
“Our data have shown that men who have germline mutations in the gene BRCA2 should be offered an annual PSA test to determine if they need to be offered an MRI and prostate biopsy.” says Eeles. “We hope that the European Association of Urology guidelines committee will consider this for a guideline recommendation after considering our data.”
In the UK, genetic testing guidelines still only recommend families with a history of breast, ovarian and prostate cancer get tested for BRCA gene mutations. In the United States, the genetic testing guidelines recommend testing when the “individual or family history suggests the possible presence of a harmful mutation in BRCA1 or BRCA2”.
This includes men with aggressive prostate cancer.
But there isn’t, however, much of a prevention plan in place in either country.
A key step along the road towards a prevention plan includes changing the public misconception that BRCA gene mutations only increase cancer risks in women, says Nangia. That could happen faster if more doctors recommended genetic testing for at-risk patients. Unfortunately, many primary care doctors feel uneasy prescribing something they may not know how to interpret.
Determining an at-risk patient can also be an involved process. It starts with establishing a comprehensive family history, explains Nangia.
At her practice in Houston, for example, they ask for patients to go back three generations on both sides. Even though you’re at a higher risk for BRCA gene mutations if an immediate family member is a carrier, a grandparent or even a great-aunt carrier can also impact your chances.
But not all medical centers are operating at this level of care. Annie Passanisi-Ruggles says that she regularly has to write in “father” on her clinic’s family history form, because they have no designated box to tick for male relatives who’ve had breast cancer.

Men carrying the BRCA2 gene who develop prostate cancer have a lower survival rate than others with the disease (Credit: Getty Images)
And if this kind of information is not being routinely collected, then it will mean many people will remain in the dark about the genetic risks they carry.
Then again, as genetic testing options have become less expensive and more commercially available, more people have been exploring their genetic health risks on their own. Direct-to-consumer genetic testing allows anyone, regardless of their family history, to test hundreds of gene variants if they so choose without a doctor’s referral for as little as $250 (£190).
Of course, these direct-to-consumer tests come with a number of downsides. If not ordered and analysed by a reliable geneticist, results can be incomplete and easily misinterpreted. And since commercial genetic testing companies are relatively unregulated, inaccuracies are common. There are also issues around how much weight should be placed on the results. Just because you carry a gene linked to a disease does not necessarily mean you will develop it.
There are, however, some genetic testing companies like Color, that offer genetic counseling along with their results. That’s a step up, says Nangia, but she’s eager for the day when regulated genetic testing with counseling is offered through all healthcare systems, regardless of history, at no cost to the patient. Interestingly enough, the National Cancer Institute has already begun research on how such testing might work.
If more genetic cancer risks like BRCA2 mutations are detected before cancers appear, then more people like Annie Passanisi- Ruggles will stay healthier longer.
“On one hand, I feel some guilt and remorse about passing the gene onto Annie, but on the other hand, I’m grateful that she knows about the gene,” says Pete. “Knowing gives her the opportunity to keep an eye out and find the right people for her care team.”
BBC
More about: cancer