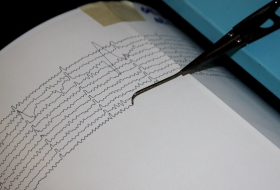
Take a good hard look at the skin of your forearm. Pinch it if you like. It may not look or feel any different from the way it did 12 hours ago, but if you were to cut or burn it, the skin would heal more than twice as fast if you injured it during daylight hours, compared to if it happened at night.
This variation in our response to insult and injury extends far beyond the skin. If you go for a seasonal flu jab, aim for a morning appointment: you’ll produce more than four times as many protective antibodies if you’re injected with it between 9am and 11am, compared to six hours later. Should you ever require heart surgery, however, the converse is true: your long-term survival prospects are significantly better if you go under the knife in the afternoon.
Indeed, wherever you look in the body, from the brain to the immune system, 24-hour rhythms that govern the activity of cells and tissues – often referred to as “circadian rhythms” – appear to dictate our physical recovery from infection and injury.
“Who we are physiologically in the daytime is different than who we are at night,” says Tami Martino, director of the Centre of Cardiovascular Investigations at the University of Guelph in Ontario, Canada, who is seeking to apply this emerging knowledge about biological timing to human and animal medicine. From cancer to cardiology, arthritis to allergies, a better understanding of these rhythms could enable drugs and interventions to be given to patients at times when they’re most likely to be effective and the least likely to cause harm. Strengthening these rhythms may also enable patients to recover faster and reduce some physical symptoms of disease.
“It is my personal belief that circadian medicine can forever change the way we manage human health,” says Martino. “It is right up there on the scale with things like gene therapy, stem cells and artificial intelligence for one of the most promising new technologies to deal with global burdens of disease.”
The idea that our physiology varies from hour to hour is, in fact, an ancient one. The Greek physician Hippocrates observed a 24-hour ebb and flow in the severity of fever. Traditional Chinese medicine also describes the vitality of different organs peaking at various times – the lungs between 3am and 5am, the heart between 11am and 1pm, the kidneys between 5pm and 7pm, and so on. There is, however, renewed interest in the effect of our internal body clocks on illness and treatments from modern medicine thanks to a growing number of recent studies.
By tweaking our urges, behaviour and biochemistry, these rhythms prepare us for regular events in our environment, which are themselves dictated by the daily cycle of light and dark. When it comes to healing, there is a good reason why it might be heightened during the day compared to at night.
“Our cells evolved to be able to heal wounds more effectively at the biological time when they are more likely to occur,” says John O’Neill, a circadian biologist at the Medical Research Council’s Laboratory of Molecular Biology in Cambridge, UK. “If you are a human, it is extremely unlikely that you will incur a major wound when you are asleep in the middle of the night, whereas during the day we are much more likely to become wounded.”
His own research has revealed that cells called fibroblasts, which help to repair tissue damage by laying down new collagen for skin cells to stick to, migrate into injured areas more rapidly during the daytime.
“We consistently found nearly a two-fold difference in wound healing simply as a function of biological time,” O’Neil says. And when they analysed data from the International Burn Injury Database, they found that people who suffer burns during the night take approximately 11 days longer to heal than those injured during the day.
Our immune system is also subject to biological rhythms that affect how it responds to infections. It might seem strange at first to vary our ability to respond to pathogens according to the time of day says Rachel Edgar, a virologist at Imperial College London. But it may have evolved this feature as a means of protecting us against over-activation of the immune system.
“If you get really big inflammatory response, you need to be able to control that otherwise it can cause a lot of damage,” says Edgar.
She has been exploring the interaction between circadian rhythms and viral infections such as herpes. In one study, she found that the herpes virus replicated 10 times as much of itself in mice that were infected at the beginning of their rest period – which, being nocturnal, falls during the early morning – compared to if they were infected at the start of their active period. Their findings suggest that the effect may be due to more than changes in the activity in the immune system. The daily rhythms of the infected cells themselves also affect the extent of a viral infection.
This evidence fits with a recent human study, which found enhanced responses to the seasonal flu vaccine when it was given in the morning compared to the afternoon. Even so, suggesting that there’s an optimal time of day to fall ill is too simplistic, cautions Edgar.
“It’s going to be different for different infectious agents,” she says.
Take sepsis, an overwhelming, and life-threatening response to an infection – it can be triggered by injecting molecules found on the surface of bacteria into the blood. If you do this to mice during their “night”, just 20% of them survive, compared to more than 90% if they’re injected during their active period.

Taking certain medicines in the morning rather than the evening may affect how effective they are (Credit: Getty Images)
The findings are opening up exciting new prospects for treating infectious diseases.
“If we know that a virus spreads to neighbouring cells at a particular time, we could potentially give antiviral therapies at the time when they are going to be most efficacious,” says Edgar. “Doing so could reduce the quantity of antivirals you need to give, which also has implications for patient compliance.”
It’s not only our response to infections that could benefit from this approach. More than half of the World Health Organization’s essential medicines – 250 drugs found in every hospital in the world – appear to hit molecular pathways regulated by internal cellular clocks, which could make them more or less effective depending on when they are taken. These include the common painkillers aspirin and ibuprofen, as well as drugs for blood pressure, peptic ulcers, asthma and cancer.
In many cases, the drugs in question have a half-life of less than six hours, which means that they don’t stay in the system long enough to work optimally if they’re taken at a sub-optimal time. For instance, the blood pressure drug, valsartan, is 60% more effective when taken in the evening, compared with first thing in the morning. Aspirin has been found to be more effective when taken in the evening, as are some antihistamine tablets for allergies such as hayfever.
ing drugs and treatments to when they’re likely to be more effective is not quite as easy as it sounds though. The cost of clinical trials soar if you have to start systematically testing for the right time of day to give a treatment. There’s also an issue around getting patients to do as they are told. Getting them to stick to a course of therapy is already tricky, but ensuring they take those drugs at a specific time is even more so.
O’Neill and others suspect that this is a key reason why, despite expressing an interest in so-called chronotherapy, drugs companies haven’t yet done a huge amount with it.
Not everyone’s circadian rhythms are the same either. Some of us are larks and some night owls. A significant proportion of the population also work night shifts, which can have its own impact on the circadian rhythm and health. And there’s currently no quick and simple test to confirm precisely where the hands of an individual’s internal clock are at any given time.
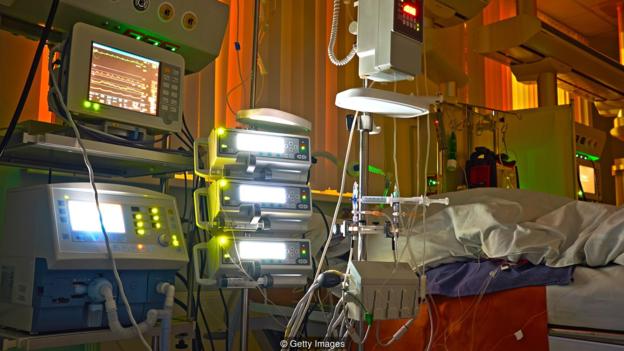
Hospitals at night often have a lot of artificial light that can not only disrupt patients’ sleep but also how their body heals (Credit: Getty Images)
Then there’s the hospital environment itself – many modern hospital buildings have small windows and dim indoor lighting that remains switched on day and night. This is problematic, because too little daylight and too much artificial light at night are disruptive to our biological rhythms and sleep.
Misaligned or flattened rhythms are a common feature of hospital patients. Compounding the problem, certain drugs, including morphine, can also alter the timing of circadian clocks, while patients’ sleep – also critical to their ability to heal – may be further disrupted by pain, worry or noise. It is leading to questions about how seriously this is impeding their recovery and survival.
Some of the strongest evidence comes from patients with heart disease. Like other tissues, the cardiovascular system has a strong circadian rhythm – our heart rate and blood pressure are lowest when we’re sleeping, but rise sharply upon waking up; our platelets, small blood fragments that help blood to form clots, are stickier during the day; while the levels of hormones like adrenaline, which constrict our blood vessels and make the heart beat faster, are also higher in the daytime. These circadian variations affect the timing of serious cardiac events, such as heart attacks.
“If you monitor people coming into emergency wards you find that heart attacks are most likely to happen between about 6am and noon compared to any other time of day or night,” says Martino. However, timing may also affect our ability to recover from heart injury.
One recent study suggested that for people undergoing heart valve replacement surgery, those who had surgery in the afternoon had half the risk of experiencing a major cardiac event during the following 500 days compared to those who underwent morning surgery. If all patients underwent afternoon surgery, this might result in one major event being avoided for every 11 patients, the researchers calculated. Other studies have indicated that, for patients recovering from a heart attack or heart surgery, those with greater exposure to daylight have higher survival rates and get out of hospital sooner.
Animal studies are providing insight into why this might be. When Martino and her colleagues exposed groups of mice either to normal or disrupted light-dark cycles after simulated heart attacks, they found significant differences in the number and type of immune cells that rallied to the heart, the amount of scar tissue – and, ultimately, survival rates. Mice whose circadian rhythms were disrupted, as they might be during a hospital stay, were more likely to die from their heart injury. Further studies have revealed differences in the type and number of immune cells that infiltrate injured heart tissue, depending on what time of day the injury occurs.
“Some intensive care units or cardiac care units will dim the lights a little bit at night, which is a bit helpful, but some don’t dim at all,” says Martino. “For example, if people come into emergency wards and there’s no beds available, they might be under bright light all night – or they might even be in a corridor all night, having had a heart attack or stroke. And so obviously their sleep and circadian rhythms are going to be profoundly disturbed during those first couple of days which are so critical for healing.”
So, what to do about it? Scheduling surgery for when the body is best placed to cope with it is one solution. For heart surgery, that might be the afternoon, but it may differ for other interventions. For instance, O’Neill’s study of wound healing suggested that more collagen is laid down when injuries are sustained during the daytime, which may be associated with greater scarring.
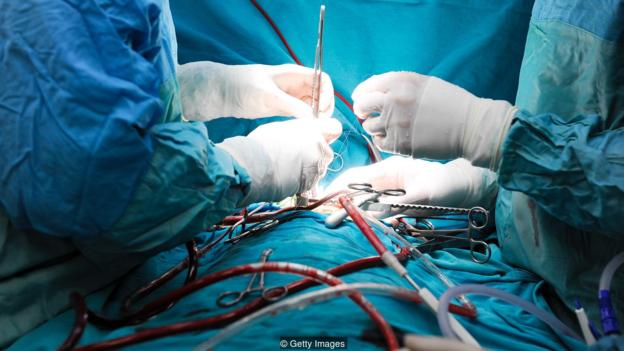
Having heart surgery in the afternoon may be better for the patient recovery but it may also leave a nastier scar (Credit: Getty Images)
“For cosmetic surgery, there might an argument for performing surgery much later – possibly in the night – because it would take longer to heal, but may result in fewer scars,” he speculates, stressing that no-one has yet tested this.
Another solution might be the installation of so-called circadian, or human-centric, lighting systems which vary in intensity and colour over the course of 24-hours, attempting to mimic natural lighting conditions outdoors. At Glostrup Hospital in Copenhagen, Denmark, doctors have been measuring the impact of such a system in the stroke rehabilitation ward. The data so far suggests that patients exhibit more robust circadian rhythms in response to the circadian lighting system, and show reduced depression and anxiety, compared with those in a section of the ward with conventional hospital lighting.
It may even be possible to design drugs that can stabilise circadian rhythms in hospital patients – or stall them for long enough to perform surgery at the optimal time for recovery. Such molecules are already being tested in animals, with promising results.
“In the future, I can envision a world where we are using a circadian pill, or the presence or absence of light to cure heart diseases,” says Martino.
Light, sleep and timing; we often take them for granted, but these three very basic things have the potential to transform health care.
More about: